From Mild Dehydration To Emergency Care: When Fluid Replacement Becomes Critical

You’ve probably experienced feeling thirsty, tired, or dizzy on a hot day, that’s your body signalling mild dehydration. But what happens when the loss of fluids becomes severe? Dehydration isn’t always harmless; in some cases, it can spiral into a medical emergency that demands immediate attention and specialised treatment. Understanding when fluid replacement becomes critical can help you respond faster and protect your health.
What Happens Inside the Body During Dehydration?
Dehydration occurs when your body loses more water and electrolytes than it takes in. This can happen due to sweating, diarrhea, vomiting, fever, or simply not drinking enough fluids. Water makes up nearly 60% of our body, and every cell depends on it to function properly.
When dehydration sets in:
- Blood volume decreases, affecting circulation.
- Heart rate increases to compensate.
- The kidneys retain water, leading to concentrated urine.
- Muscles and organs receive less oxygen.
If left untreated, these internal changes can quickly lead to shock, confusion, or even organ failure.
Common Causes of Dehydration
Some causes are everyday situations, while others can be medical emergencies. Here are the most common:
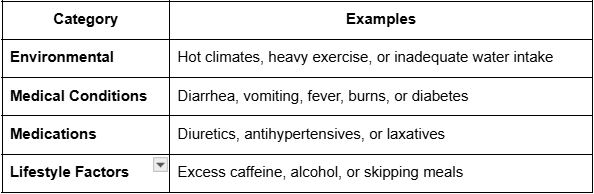
Even mild dehydration can cause fatigue and brain fog, but prolonged dehydration requires medical evaluation.
Signs You Might Be Dehydrated
Recognising the symptoms early can prevent complications. Look out for these signs:
- Dry mouth or cracked lips
- Dizziness or light-headedness
- Dark yellow urine or reduced urination
- Fatigue and muscle cramps
- Increased heart rate
- Dry skin or lack of sweat
Severe dehydration may present with confusion, fainting, rapid breathing, or low blood pressure, all of which signal a need for emergency care.
From Oral Rehydration to IV Fluids: Different Levels of Treatment
The right treatment depends on the severity of the dehydration.
1. Mild Dehydration:
Often managed with oral rehydration solutions or water intake. Electrolyte-rich fluids, such as coconut water or rehydration drinks, help restore balance.
2. Moderate Dehydration:
If vomiting or diarrhea persists, doctors may recommend IV fluids to replace lost electrolytes and stabilise blood circulation.
3. Severe Dehydration or Shock:
This stage needs immediate hospital care. Fluids are given intravenously, often containing saline or specialised solutions that balance sodium and potassium.
In critical cases where blood plasma needs restoration, Flexbumin 20% Injection 100ml use may be advised under medical supervision to help restore lost proteins and improve fluid balance.
Role of Human Albumin in Fluid Replacement
One of the vital components used in advanced dehydration management is Human Albumin. This naturally occurring protein helps maintain the balance between fluids inside and outside blood vessels. When dehydration leads to low blood volume or pressure, Human Albumin can help:
- Improve circulation
- Maintain stable blood pressure.
- Transport essential substances like hormones and drugs
Doctors use it cautiously in cases where standard fluid therapy isn’t enough to restore stability.
When Dehydration Becomes a Medical Emergency
Sometimes, dehydration develops silently until symptoms worsen. It becomes critical when:
- There’s continuous vomiting or diarrhea
- You cannot retain fluids.
- You experience confusion or fainting.
- Blood pressure drops drastically.
- Urine output nearly stops.
These symptoms may indicate severe electrolyte imbalance or hypovolemic shock, both requiring urgent fluid replacement and monitoring in a hospital.
At-Risk Groups: Who Needs to Be Extra Careful?
Certain people are more prone to dehydration and may need proactive care:
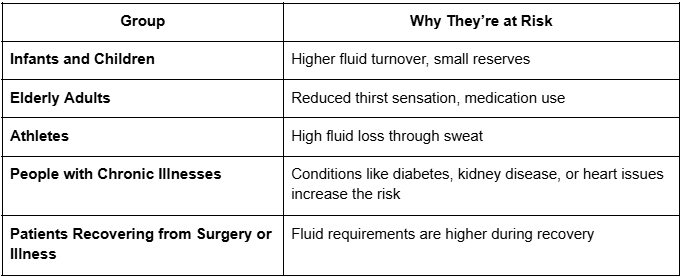
Practical Tips to Prevent Severe Dehydration
While medical care is crucial for serious cases, daily prevention is the best defence.
1. Stay hydrated throughout the day. Carry a water bottle and take small sips frequently.
2. Eat water-rich foods. Fruits like watermelon, cucumber, and oranges contribute to fluid intake.
3. Balance electrolytes. Include oral rehydration salts or coconut water after exercise or illness.
4. Limit dehydrating substances. Avoid excess caffeine and alcohol.
5. Be mindful in hot climates. Wear light clothes and take breaks during physical activity.
6. Monitor early warning signs. Dark urine or dry lips mean it’s time to drink more fluids.
The Link Between Dehydration and Other Conditions
Dehydration can worsen several underlying conditions, such as kidney disorders, diabetes, or heatstroke. Chronic dehydration also affects skin elasticity, digestion, and heart health. It’s not just about water loss, it’s about how your body maintains internal balance. That’s why doctors emphasise hydration as part of a larger wellness routine.
Takeaways
Staying hydrated may sound simple, but it’s one of the most effective ways to protect your health. Dehydration doesn’t always show up dramatically; sometimes, it begins with mild symptoms that go unnoticed. Recognising early warning signs, drinking fluids consistently, and seeking help when necessary can prevent serious complications. Whether through natural hydration or medical intervention, maintaining a balanced fluid intake is vital for every stage of life.
